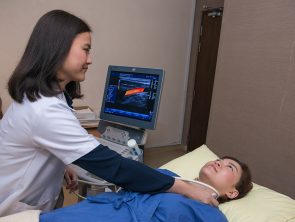
Doppler Ultrasound
A Doppler ultrasound is a noninvasive test that can be used to estimate the blood flow through your blood vessels by bouncing high-frequency sound waves (ultrasound) off circulating red blood cells.
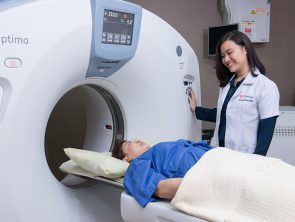
CT Angiogram
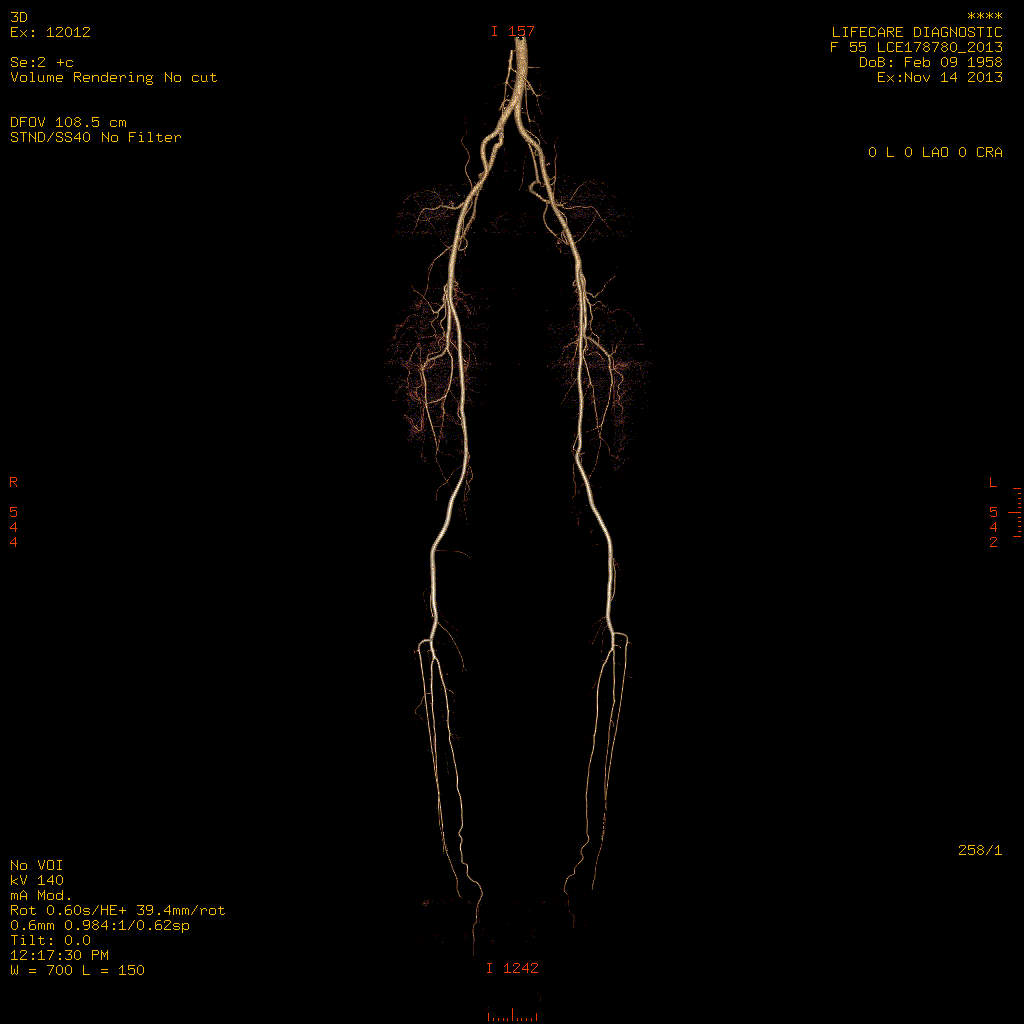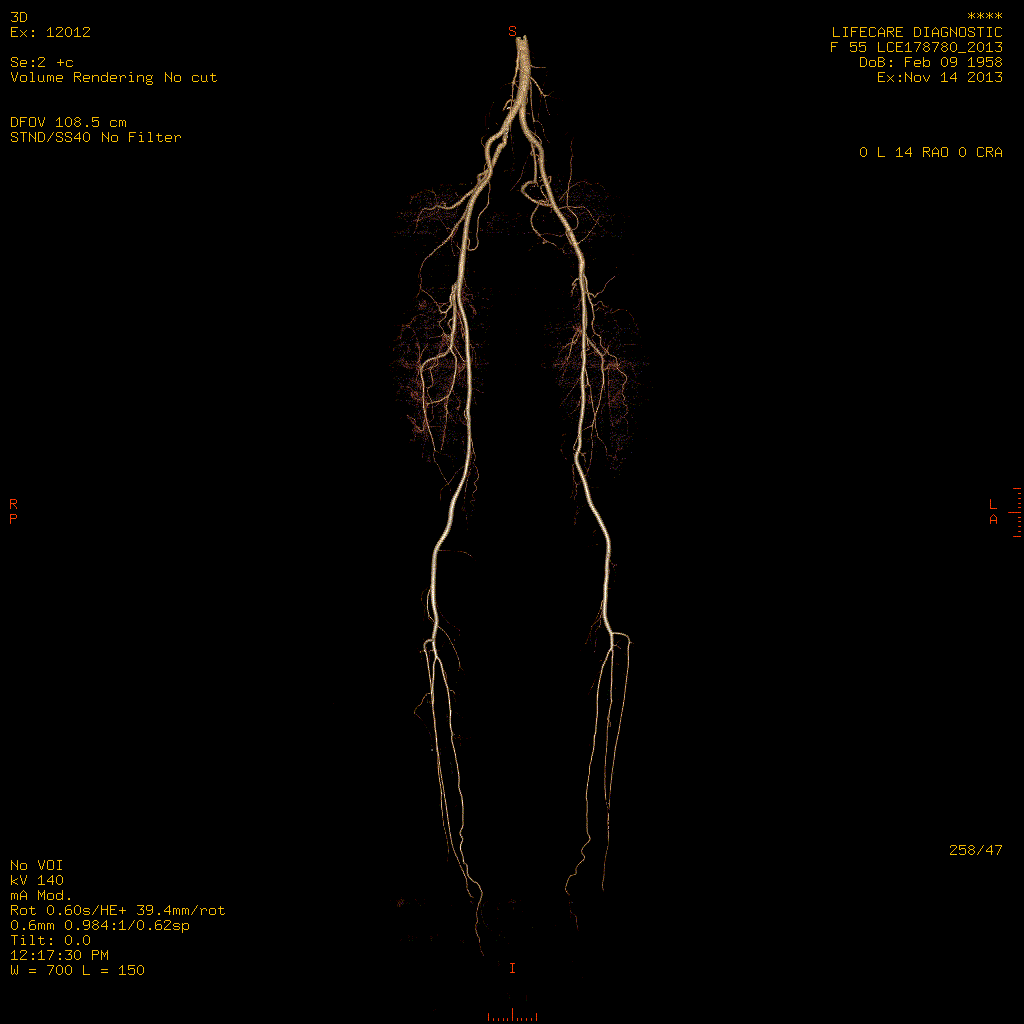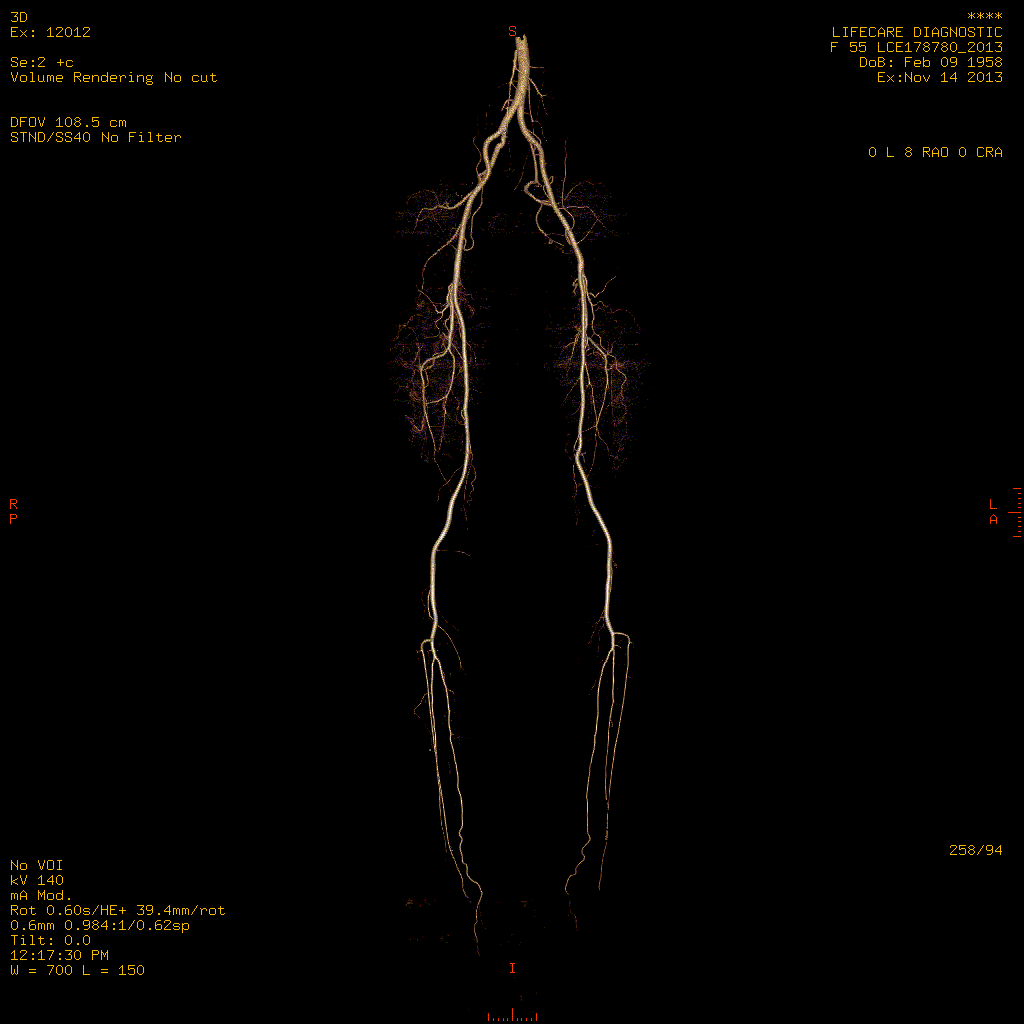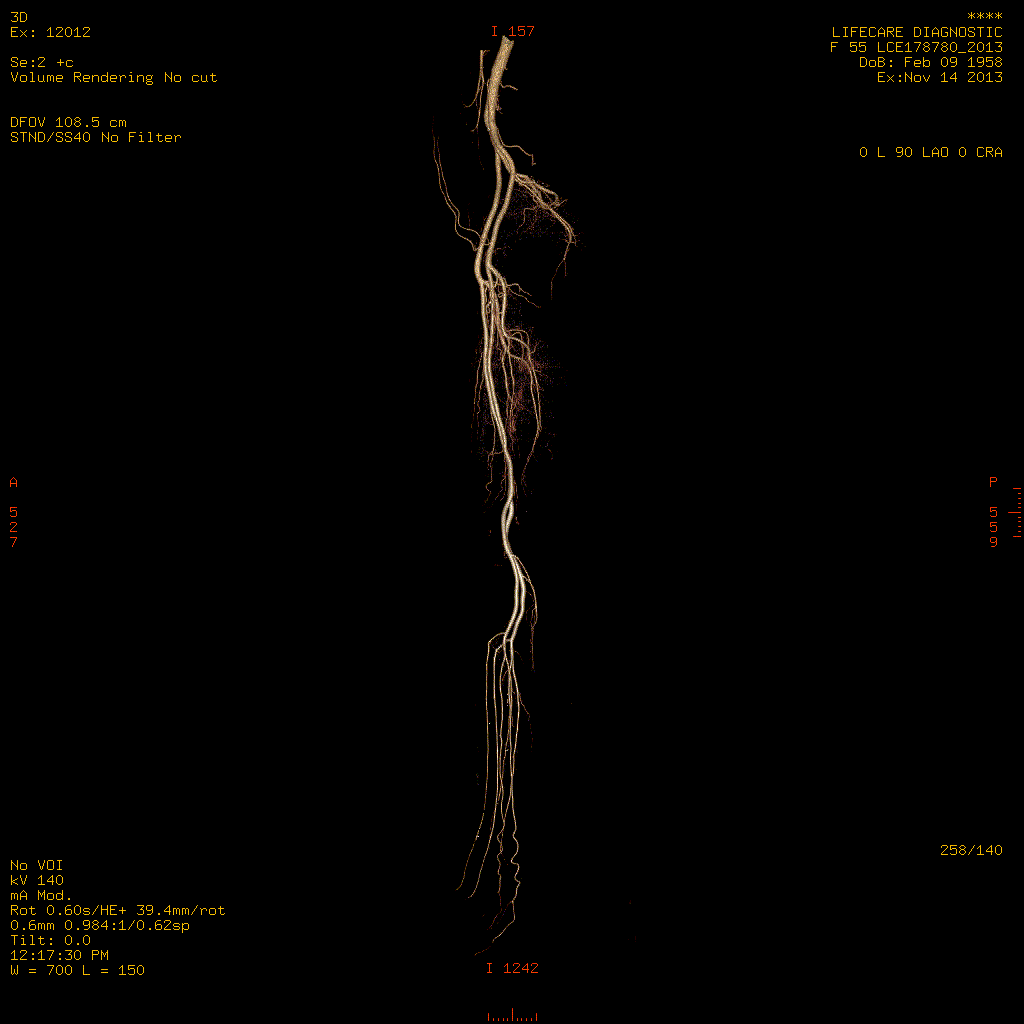
CT Angiography is a safe outpatient procedure that uses specially designed x-rays and intravenous contrast to see the detailed anatomy of the blood vessels throughout the body. It is most frequently utilized in the evaluation of arteries in the head, neck, chest, abdomen and legs. Coronary CT angiography refers to the scanning procedure of the arteries of the heart i.e. those involved in ischaemic heart disease like heart attacks.
How can I prepare for CT Angiogram Test?
You need only to fast for about 4 hours before the scan. Please refrain from caffeinated drinks e.g. coffee or tea on the day of the examination.
How long does a CT Angiogram take?
Although the actual heart scanning takes only 5-8 seconds, the whole scanning procedure may take about 15-20 minutes from preparation to completion. You would be able to leave immediately after the procedure and would be able to resume normal activities.
MR Angiography
Magnetic resonance angiography (MRA) is a non-invasive medical imaging test that uses a magnetic field and radio waves frequency to produce detailed images of the major arteries within the body, such as the brain, heart & other body parts. MR angiography does not use ionizing radiation (x-rays). MRA may be performed with or without contrast material.
How should I prepare?
How is the procedure performed?
What conditions should I inform my doctor of?
Women should inform their doctor or radiographer if there is any possibility that they are pregnant.
X-Ray
An x-ray (radiograph) is a noninvasive medical test that helps physicians diagnose and treat medical conditions. Imaging with x-rays involves exposing a part of the body to a small dose of ionizing radiation to produce pictures of the inside of the body. X-rays are the oldest and most frequently used form of medical imaging.
We can perform an x-ray for any bone in the body, including the hand, wrist, arm, elbow, shoulder, spine, pelvis, hip, thigh, knee, leg (shin), ankle or foot.
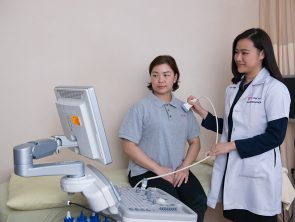
Ultrasound scan
Ultrasound imaging uses sound waves to produce pictures of muscles, tendons, ligaments and joints throughout the body. It is used to help diagnose sprains, strains, tears, and other soft tissue conditions. Ultrasound is safe, noninvasive, and does not use ionizing radiation.
This procedure requires little to no special preparation. Leave jewellery at home and wear loose, comfortable clothing. You may be asked to wear a gown.
MRI
MRI is a non-invasive medical imaging test that uses a magnetic field and radio waves frequency to produce detailed pictures of organs, soft tissues, bones, joints and other internal body structures. MRI does not use ionizing radiation (as used in x-rays and CT scans).
How should I prepare?
How is the procedure performed?
What conditions should I inform my physician of?
Bone Mineral Densitometry
Bone mineral densitometry, also called dual-energy x-ray absorptiometry or DEXA, uses a very small dose of ionizing radiation to produce pictures of the inside of the body (usually the lower spine and hips) to measure bone loss. It is commonly used to diagnose osteoporosis and assess an individual’s risk for developing fractures. DEXA is simple, quick and noninvasive. It’s also the most accurate method for diagnosing osteoporosis.
Carotid Intima-Media Thickness (Carotid IMT) Ultrasound
Measurement of carotid IMT in the carotid artery with ultrasound is a non-invasive, sensitive, and reproducible technique for identifying and quantifying subclinical vascular disease and for evaluating Cardiovascular Disease (CVD) risk – heart attacks and strokes and also to predict future cardiovascular disease (heart attacks and strokes) risk.
Who should get a Carotid IMT Ultrasound Test?
Coronary Heart Disease (CVD) risk factors (Risks for developing heart attacks and strokes):
When does atherosclerosis starts?
The atherosclerotic vascular disease begins in childhood and progresses over decades. Symptomatic, clinical cardiovascular disease (CVD) events generally occur when atherosclerosis progresses to flow-limiting disease that causes ischemia, or when a thrombus forms on an existing plaque as a result of rupture or erosion.
Although not everyone with underlying atherosclerotic plaque will experience a clinical CVD event, the greater the degree of subclinical atherosclerosis, the greater the risk for future cardiovascular events.
To prevent death and morbidity from CVD, there is great interest in identifying asymptomatic patients at high risk who would be candidates for more intensive, evidence-based medical interventions that reduce CVD risk.
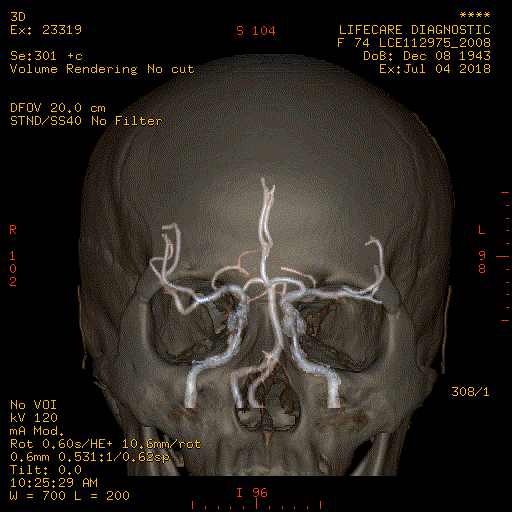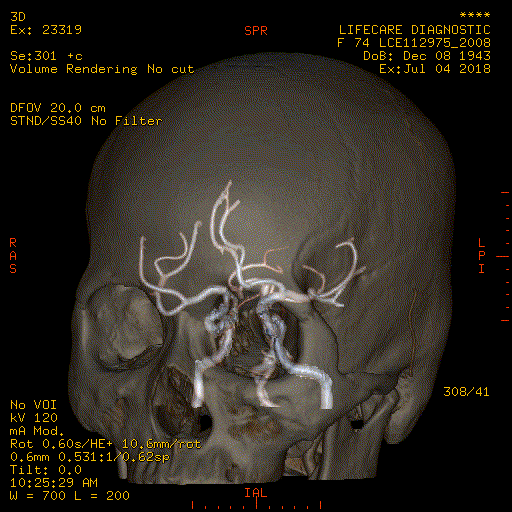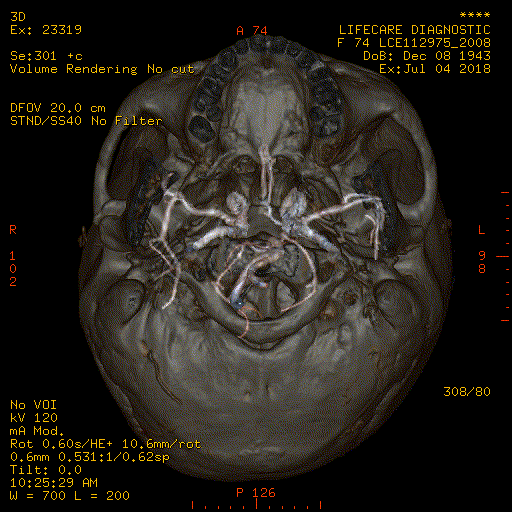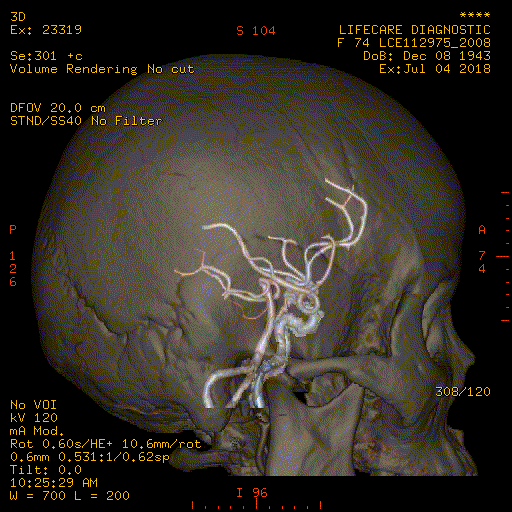
CT Cerebral Angiogram
In CT Angiography (CTA), computed tomography uses a contrast material to produce pictures of blood vessels in the brain.
What are some common uses of the procedure?
Doctors use the procedure to detect or confirm abnormalities within the blood vessels in the brain, including:
How should I prepare for the procedure?
You should wear comfortable, loose-fitting clothing. You may be given a gown to wear during the procedure.
Metal objects including jewellery, eyeglasses, dentures and hairpins may affect the CT images and should be left at home or removed prior to the procedure.
You may also be asked to remove hearing aids and removable dental work. You may be asked not to eat or drink anything for several hours beforehand, especially if a contrast material will be used in the procedure. You should inform the doctor of any medications you are taking and if you have any allergies, especially to contrast materials.
Also, inform the doctor of any recent illnesses or other medical conditions, and if you have a history of heart disease, asthma, diabetes, kidney disease or thyroid problems. Any of these conditions may increase the risk of an unusual adverse effect.
Women should always inform the doctor or technologist if there is any possibility that they are pregnant.
MRI Brain/ MRI Carotids Angiography/ MRI Cerebral Angiography
MRI is a non-invasive medical imaging test that uses a magnetic field and radio waves frequency to produce detailed pictures of organs, soft tissues, bone and other internal body structures.
MRI brain produces detailed images of the brain & the brain stem. MRI does not use ionizing radiation (as used in x-rays and CT scans).
How should I prepare?
How is the procedure performed?
The radiographer begins by positioning you on the MRI examination table. Straps and pillows may be used to help you maintain the correct position and to hold still during the examination.
After positioning you, the radiographer will offer you earplugs to reduce the noise of the MRI scanner, which produces loud thumping and humming noises during imaging. These noises are harmless. Then, the radiographer will enter a separate room where the radiographer operates the MRI machine and monitor your examination. The radiographer will be able to see, hear and speak with you at all times.
The table will move slowly through the machine as the MRI scan is performed. When images are being recorded, you will hear a thumping and humming sound. Please remain still while the images are being recorded. It is normal for the area of your body being imaged to feel slightly warm. If it bothers you, please notify the radiographer.
When the examination is completed, you will be asked to wait until the radiologist verifies that the images are of good quality for accurate interpretation. Though the scanning itself causes no pain, there may be some discomfort from having to remain still for several minutes.
What conditions should I inform my doctor of?
Women should always inform the doctor or radiographer if there is any possibility that they are pregnant. MRI has been used for scanning patients since the 1980s with no reports of any ill effects on pregnant women or their babies. However, because the baby will be in a strong magnetic field, pregnant women should not have this examination unless the potential benefit from the MRI exam is assumed to outweigh the potential risks.
If you have a hard time staying still, are claustrophobic or have chronic pain, you may find an MRI examination to be stressful. The radiographer, under the direction of a doctor, may offer you some sedation prior to the scheduled examination to help you tolerate the MRI scan procedure.
Breast Ultrasound
An ultrasound machine uses high-frequency sound waves to produce images of the internal structures of the human body. The Ultrasound scan is done to look at the internal organs of the breast.
The primary use of breast ultrasound today is to help diagnose breast abnormalities detected by a physician during a physical exam and to characterize potential abnormalities seen on mammography.
The general guide for Breast Ultrasound
Mammography
Mammography is a safe low-dose x-ray examination of the breasts which is used to detect and diagnose breast diseases. The x-ray film is called the mammogram. Screening mammography is used as a preventive measure for women who have no symptoms of breast disease.
Why should I have a Mammography?
Women in Malaysia have a 1 in 19 chance of getting breast cancer in their lifetime. Mammography is used to detect breast cancer early before it can be felt, and thus have a better chance of surviving the disease. Along with a mammogram, an actual breast lump must be assessed by a doctor. (Source: BreastHealth Information Centre, www.radiologymalaysia.org)
Besides, The American Cancer Society recommends that all women aged 40 and over have a screening mammography every year as part of a breast health programme. This also includes monthly breast self-examinations and an annual breast examination by a healthcare professional.
Women who have had breast cancer or breast problems or with a family history of breast cancer are at a higher risk for breast cancer. They may need to start screening at a younger age or more frequently as advised by their doctor.
How is a Mammography done?
A female radiographer will place each breast in turn on the mammography unit and use a paddle to compress the breast. The breast is compressed to spread the tissue apart. This allows the maximum amount of tissue to be imaged and reduces radiation dose. The flatter the breast, the better the image. The compression will only last for a few seconds. It is uncomfortable but should not be painful. The radiographer will step behind a screen and take the x-ray images. As a rule, two views in different positions of each breast are taken.
How can I prepare for the Mammography?
Do not schedule your mammography for the week before your period as your breasts are usually tender during this time. The best time is one week after your period. Do not apply deodorant, lotion and talcum powder under your arms or on your breasts on the day of examination. They may appear on the film as calcium spots.
Always inform the doctor or radiographer if there is any possibility that you are pregnant. Describe any breast symptoms or problems before performing the exam.
How long does a Mammography take?
The mammography takes only a few seconds. However, the total time taken to prepare and position the patient for the x-ray examination takes about 20-30 minutes.
Are there any possible complications?
Today’s mammography units use very low doses of radiation to produce high-quality mammograms, making this a very safe procedure.
The radiation dose from a mammogram is about the same as we receive from background radiation in three months.
False-positive mammograms: 5-10 per cent of screening mammogram results are abnormal and require more testing (more mammograms, ultrasound or biopsy) and most of the follow-up tests confirm that no cancer was present. It is estimated that a woman between the age of 40 and 49, who has yearly mammograms will have about a 30 per cent chance of having a false-positive mammogram at some point in that decade, and about a 7-8 per cent chance of having a breast biopsy within the 10-year period. The estimate for false-positive mammograms is about 25 per cent for women in the age group of 50 or over.
What are the limitations of Mammography?
Not all cancers of the breast can be seen on mammography. The false-negative rate is 10-15 per cent. Because some breast cancer is hard to visualize, a radiologist may want to compare your mammogram to images from previous examinations. You should always tell the doctor about a suspicious lump even if you have had a recent mammogram done.
Breast implants can also obstruct accurate mammogram readings because they can block a clear view of the breast tissues.
The general guide for Mammography
Exercise Stress Test
This is a well-established and common heart investigation that has been in use for several decades and is used primarily in the evaluation of ischaemic heart disease. It is also known as Treadmill Exercise Stress Test. However, it is also conducted in the evaluation of a number of other heart problems.
How can I prepare for my Exercise Stress Test?
How long is the Exercise Stress Test?
The duration depends very much on the target heart rate and the time it takes to achieve it. In general, it would about 30 minutes from preparation to completion of the test.
Who should avoid Exercise Stress Test?
The Exercise Stress Test should not be done on selected groups of people as listed below:
What does it mean if my test is positive?
A positive result suggests the possibility of coronary artery disease (CAD). The doctor will interpret this test whilst taking into account the pre-test probability of disease. If there is a strong suspicion, more definitive tests eg. CT Coronary Angiography may be advised.
Does a negative test mean that I am free from any heart disease?
Stress test estimates the probability of disease. The specificity of this test (ie. the likelihood of a negative test when one is truly free of disease) is about 70-80%. Therefore, a negative test does not rule out heart disease completely. Again, the interpretation of this test depends on your baseline probability of disease.
As mentioned, this test detects only severe coronary artery obstructions (>70%). As we know today, most heart attacks occur not from severe narrowings but the mild to moderate ones. Hence, although it is a good test to screen for the presence of CAD, there are limitations and it is never definitive.
Carotid Intima-Media Thickness (Carotid IMT) Ultrasound
Measurement of carotid IMT in the carotid artery with ultrasound is a non-invasive, sensitive, and reproducible technique for identifying and quantifying subclinical vascular disease and for evaluating Cardiovascular Disease (CVD) risk – heart attacks and strokes and also to predict future cardiovascular disease (heart attacks and strokes) risk.
Who should get a Carotid IMT Ultrasound Test?
Coronary Heart Disease (CVD) risk factors (Risks for developing heart attacks and strokes):
When does atherosclerosis starts?
The atherosclerotic vascular disease begins in childhood and progresses over decades. Symptomatic, clinical cardiovascular disease (CVD) events generally occur when atherosclerosis progresses to flow-limiting disease that causes ischemia, or when a thrombus forms on an existing plaque as a result of rupture or erosion.
Although not everyone with underlying atherosclerotic plaque will experience a clinical CVD event, the greater the degree of subclinical atherosclerosis, the greater the risk for future cardiovascular events.
To prevent death and morbidity from CVD, there is great interest in identifying asymptomatic patients at high risk who would be candidates for more intensive, evidence-based medical interventions that reduce CVD risk.
Echocardiography
This is a common non-invasive investigation tool for heart conditions. It applies ultrasound waves to generate images of the structures of the heart. It allows real-time visualization of the heart and the large blood vessels connected to it.
With the use of Doppler ultrasound technology, we are also able to interrogate the function of heart valves, derive blood pressures of different heart chambers and assess the functions of the heart.
How do I prepare for an Echocardiography examination?
There is no special preparation needed for this painless, non-invasive procedure. Clothing from the upper body is removed and covered by a gown or sheet to keep you comfortable and maintain the privacy of females. The patient then lies on an examination table.
How is an Echocardiography examination done?
ECG electrodes are attached to the body to allow the timing of the heart events to the ECG cycle. A transducer (a probe that transmits and receives ultrasonic waves) is placed over the chest or region of interest. A colourless gel is applied to the probe before scanning to improve the image quality.
The echo technologist or cardiologist would acquire images from different parts of the chest to obtain views from different angulations. You may be advised to assume certain body positions for better imaging of the different heart or non-heart structures.
How long does an Echocardiography examination take?
An evaluation of a normal heart generally takes about 10-15 minutes. However, a more detailed interrogation of abnormal findings may take a bit longer.
What information can I obtain from an Echocardiography examination?
(Heart CT Scan) Calcium Score
Calcium is a marker of coronary artery disease, the amount of calcium detected on a heart CT scan is a helpful diagnostic tool. The findings of heart CT are expressed as a calcium score. Another name for this test is Coronary Artery Calcium Scoring.
CT Scan is a noninvasive, painless medical test that helps doctors diagnose and treat medical conditions. A heart CT Scan is a non-invasive way of obtaining information about the location and extent of calcified plaque in the coronary arteries – the vessels that supply oxygen-containing blood to the heart wall.
Plaque is a build-up of fat and other substances, including calcium, which can, over time, narrow the arteries or even close off blood flow to the heart. The result may be painful angina in the chest or a heart attack.
How should I prepare for the procedure?
No special preparation is necessary in advance of a heart CT scan. You may continue to take your usual medications but should avoid caffeine and smoking for 4 hours before the exam. If your heart rate is 90 beats a minute or higher, you may be given a drug to slow the rate in order to obtain accurate CT images.
You should wear comfortable, loose-fitting clothing to your exam. You may be given a gown to wear during the procedure. Metal objects including jewellery, eyeglasses, dentures and hairpins may affect the CT images and should be left at home or removed prior to your exam. You may also be asked to remove hearing aids and removable dental work.
Women should always inform the doctor or technologist if there is any possibility that they are pregnant.
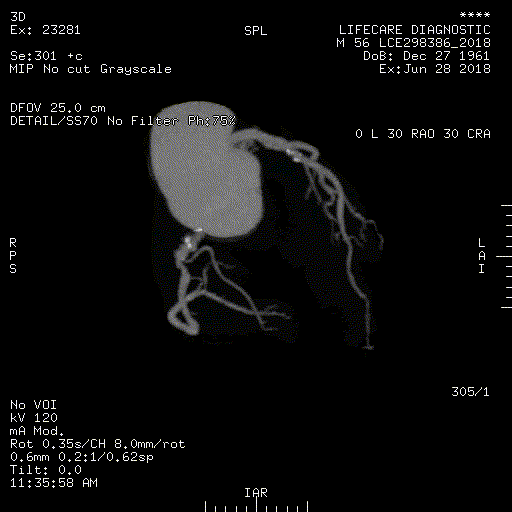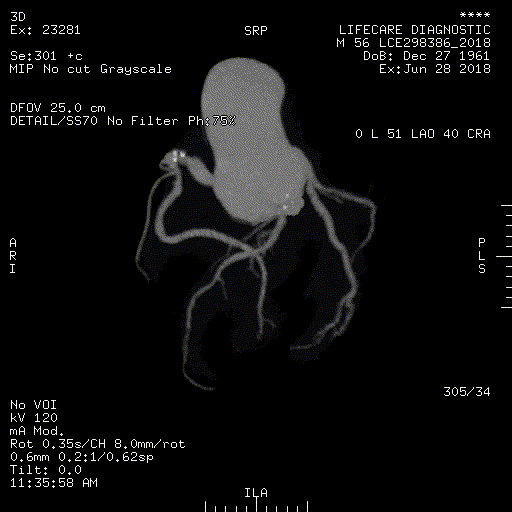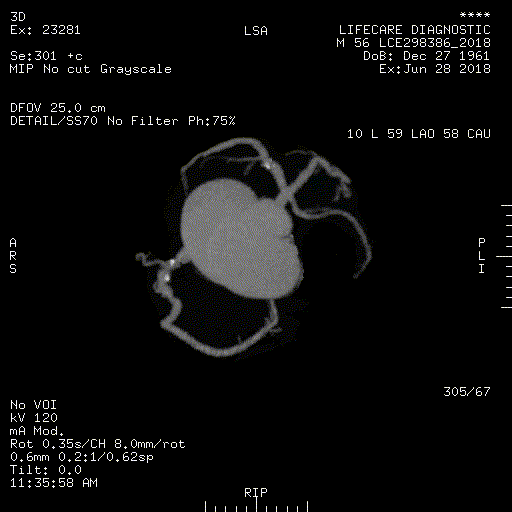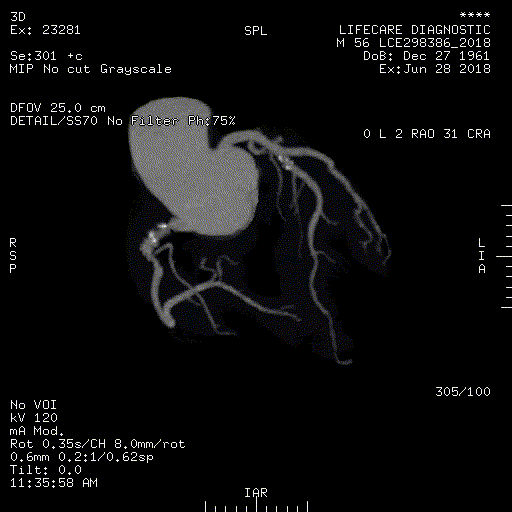
Non-invasive CT Coronary Angiography
CT Angiography is a safe outpatient procedure that uses specially designed x-rays and intravenous contrast to see the detailed anatomy of the blood vessels throughout the body. It is most frequently utilized in the evaluation of arteries in the head, neck, chest, abdomen and legs. Coronary CT angiography refers to the scanning procedure of the arteries of the heart i.e. those involved in ischemic heart disease like heart attacks.
How safe is a CT Coronary Angiography scan?
There are certainly radiation issues with this modality. The effective dose is almost similar to that of an invasive heart catheterization (5-8 mSv). Contrast use would entail the risk of allergic reaction in a small proportion of the population. Therefore, not all persons would benefit from this test. Please discuss with the doctor the proper indications and the risk-benefit analysis of performing such a scan.
Who should have a CT Coronary Angiography scan?
Coronary CT Angiography is ordered by the doctor if there is a need to establish the presence of significant coronary artery disease. It may be indicated if initial heart screening tests e.g. Stress ECG tests or nuclear heart scans are abnormal. It is also used for the follow-up of patients after coronary angioplasty and stenting, post coronary bypass grafting surgery.
How is the CT Coronary Angiography done?
Intravenous access needs to be obtained. You will be asked to lie down on the CT scanning table. Breath-holding instructions will be given. Often the whole heart can be imaged within 5 heartbeats. Contrast injection is necessary and sometimes, you may need medication to slow down the heart rate.
Following image acquisition, our radiographer and doctor will process and report on the images. The results will be discussed with you.
How can I prepare for a CT Coronary Angiography scan?
You need only to fast for about 4 hours before the scan. Please refrain from caffeinated drinks e.g. coffee or tea on the day of the examination.
How long does a CT Coronary Angiography Scan take?
Although the actual heart scanning takes only 5-8 seconds, the whole scanning procedure may take about 15-20 minutes from preparation to completion. You would be able to leave immediately after the procedure and would be able to resume normal activities.
How good is a CT Coronary Angiography?
The most advanced multi-detector CT today is a 128-detector row scanner. By using very fast gantry rotation speed and large volume detector coverage, we are able to obtain detailed visualization of the coronary tree. This is a very promising new technology. The latest data are reporting excellent results.
A recent study, presented in March 2005 at the annual meeting of the American College of Cardiology, compared the capacity of 128-slice heart CT versus coronary angiography to detect significant coronary artery stenosis (defined as more than 50 per cent lumen diameter reduction). 30 patients with stable angina or acute coronary syndrome were enrolled in the study; individuals unable to hold their breath for less than 15 seconds were excluded from the study. The heart was scanned following intravenous injection of contrast material and analyzed by two observers who were not aware of the results obtained from invasive angiography.
Most patients received a beta blocker before the study, and all coronary arteries were compared between coronary CT and selective angiography. Compared with selective angiography, 128-channel heart CT showed a sensitivity of 96% and specificity of 89% when detecting significant stenosis (narrowing). The authors concluded that 128-channel heart CT could reliably detect significant coronary stenosis in patients with stable angina or acute coronary syndrome (Source: Mollet, et. al., presentation #1054-83, ACC ‘05).
A more recent analysis (Hoffman et al., JAMA 2005; 293:2471-2478) showed an MDCT sensitivity of 95% and specificity of 98%.
Is CT Coronary Angiography an alternative to Catheter Angiography?
Heart catheterization remains the gold standard for diagnosing coronary artery disease. However, the setback with this approach lies in the fact that it is invasive, requires a longer hospital stay and has complications, e.g., bleeding, and pain and it costs more.
Compared to Catheter Angiography, CT Angiography is a less invasive and more patient-friendly procedure. Although contrast is injected through an artery in Catheter Angiography, CT Angiography contrast is injected into a vein which is technically less difficult and has a very low risk of complication. As a result, the patients typically leave immediately following the procedure and can resume normal activities.
Heart CT also offers the advantage of being able to visualize atherosclerotic plaque composition. Heart catheterization only opacifies the arterial lumen.
What does it mean if my scan is positive or equivocal?
Your scan would be able to tell if there is an atherosclerotic narrowing of the coronary arteries. It can also estimate the degree of obstruction. Based on these findings, the cardiologist will advise you further on the subsequent management.
Sometimes, the presence of excessive calcium or certain stents in the arteries may interfere with the proper interpretation of the scans and hence reduce their accuracy.
Does a negative scan mean that I am free from Coronary Arterial Disease?
Having a normal scan is an excellent result. The negative predictive value of a 128-slice MDCT Coronary Angiography is about 99-100%. This means that if the scan result is normal, the likelihood of this being true is nearly 100%.
Kidney, Ureter & Bladder (KUB) Ultrasound
The KUB Ultrasound, or Renal Ultrasound, will use high-frequency sound waves transmitted through a transducer (probe) to visualize and assess your kidneys, ureters (small muscular tubes that join the kidneys with the bladder) and urinary bladder.
How can I prepare?
No fasting is needed. You will need to keep a full bladder for the ultrasound of the pelvis.
CT Scan Urography
A computerized tomography (CT) urography is an imaging exam used to evaluate your urinary tract, including your kidneys, your bladder and the tubes (ureters) that carry urine from your kidneys to your bladder.
How should I prepare for the procedure?
You should wear comfortable, loose-fitting clothing to your exam. You may be given a gown to wear during the procedure. Metal objects including jewellery, eyeglasses, dentures and hairpins may affect the CT images and should be left at home or removed prior to your exam. You may also be asked to remove hearing aids and removable dental work. You may be asked not to eat or drink anything for several hours beforehand, especially if a contrast material will be used in your exam.
You should inform the doctor of any medications you are taking and if you have any allergies, especially to contrast materials. Also, inform the doctor of any recent illnesses or other medical conditions, and if you have a history of heart disease, asthma, diabetes, kidney disease or thyroid problems. Any of these conditions may increase the risk of an unusual adverse effect.
Women should always inform the doctor or technologist if there is any possibility that they are pregnant.
Urinary Flow Assessment – Uroflowmetry
Uroflowmetry is a test that measures the volume and speed of urine released from the body, and how long the release takes.
The indications for Uroflow Test:
How can I prepare for Uroflowmetry Test?
Fatty Liver & Liver Fibrosis Test
Specialized ultrasound machine for the liver. It measures fibrosis (scarring) and steatosis (fatty change) in your liver.
The result is displayed as a number, or score, rather than a picture, which tells your doctor how much liver scarring you have.
The test will help the doctors learn more about your liver disease. It can be used alone or with other tests such as blood tests, imaging scans, and biopsies.
Benefits of Fatty Liver & Liver Fibrosis Test
What happens during the scan?
How can I prepare for the Fatty Liver & Liver Fibrosis Test?
Abdominal & Pelvic Ultrasound
An ultrasound machine uses high-frequency sound waves to produce images of the internal structures of the human body. The Abdomen and Pelvic Ultrasound scan is done to look at the internal organs, namely, the liver, spleen, gallbladder, pancreas, kidneys, bladder, uterus and ovaries in a woman and the prostate in a man.
How is an Abdominal & Pelvic Ultrasound is done?
You will be taken to an ultrasound suite which is dimly lit. You will have to lie down on the ultrasound couch and uncover your abdomen. The transparent gel is applied to your abdomen. A transducer connected to the scanning machine is placed on your abdomen and moved around to see the respective organs. The transducer sends sound waves into your body.
These sound waves bounce off an organ like an echo. The ‘echo’ is sent to a machine that records the results on film and on a computer. You will not hear or feel high-frequency sound waves. There may be a slight discomfort from pressure as the radiologist guides the transducer over your abdomen. You will be asked to remain as still as you can and to hold your breath when the images are taken.
How can I prepare for the Abdominal & Pelvic Ultrasound?
You need to fast for six hours prior to the scan. You will need to keep a full bladder for the ultrasound of the pelvis.
How long is an Abdominal & Pelvic Ultrasound?
It will take about 15 – 30 minutes depending on the complexity of the scan.
Abdomen and Pelvis CT Scan
Computed tomography (CT) of the abdomen and pelvis is a diagnostic imaging test used to help detect diseases of the small bowel, colon, liver, gallbladder, pancreas, kidneys, uterus, prostate and other internal organs CT scanning is fast, painless, noninvasive and accurate, performed with intravenous contrast material after the ingestion of oral contrast
How should I prepare for the procedure?
You should wear comfortable, loose-fitting clothing to your exam. You may be given a gown to wear during the procedure.
Metal objects including jewellery, eyeglasses, dentures and hairpins may affect the CT images and should be left at home or removed prior to your exam.
You may also be asked to remove hearing aids and removable dental work. You may be asked not to eat or drink anything for several hours beforehand, especially if a contrast material will be used in your exam. You should inform your physician of any medications you are taking and if you have any allergies, especially to contrast materials.
Also, inform the doctor of any recent illnesses or other medical conditions, and if you have a history of heart disease, asthma, diabetes, kidney disease or thyroid problems. Any of these conditions may increase the risk of an unusual adverse effect.
Women should always inform the doctor or technologist if there is any possibility that they are pregnant.
Neck CT Scan
CT scans of the neck provide more details on neck injuries, tumours, and other diseases than other types of X-ray. CT scan also shows bone, soft tissues, and blood vessels in the same pictures. No special preparation needed prior to the test.
How Should I Prepare For The Procedure?
You should wear comfortable, loose-fitting clothing to your exam. You may be given a gown to wear during the procedure.
Metal objects including jewelry, eyeglasses, dentures and hairpins may affect the CT images and should be left at home or removed prior to your exam.
You may also be asked to remove hearing aids and removable dental work. You may be asked not to eat or drink anything for several hours beforehand, especially if a contrast material will be used in your exam. You should inform your physician of any medications you are taking and if you have any allergies, especially to contrast materials.
Also, inform the doctor of any recent illnesses or other medical conditions, and if you have a history of heart disease, asthma, diabetes, kidney disease or thyroid problems. Any of these conditions may increase the risk of an unusual adverse effect.
Women should always inform the doctor or technologist if there is any possibility that they are pregnant.
Pelvic Ultrasound
Ultrasound scan of the pelvis uses sound waves to produce pictures of the structures and organs in the lower abdomen and pelvis.
How is a Pelvic Ultrasound done?
You will be taken to an ultrasound room which is dimly lit. You will have to lie down on the ultrasound couch and uncover your abdomen. The transparent gel is applied to your abdomen. A transducer connected to the scanning machine is placed on your abdomen and moved around to see the respective organs. The transducer sends sound waves into your body.
These sound waves bounce off an organ like an echo. The ‘echo’ is sent to a machine that records the results on film and on a computer. You will not hear or feel high-frequency sound waves. There may be a slight discomfort from pressure as the radiologist guides the transducer over your abdomen. You will be asked to remain as still as you can and to hold your breath when the images are taken.
How can I prepare for the Pelvic Ultrasound?
No fasting is needed. You will need to keep a full bladder for the ultrasound of the pelvis.
How long does a Pelvic Ultrasound take?
It will take about 10 – 15 minutes depending on the complexity of the scan.
Prostate MRI
MRI is a non-invasive medical imaging test that uses a magnetic field and radio waves frequency to produce detailed pictures of organs, soft tissues, bone and other internal body structures. MRI of the prostate produces detailed images of the prostate gland. MRI does not use ionizing radiation.
How should I prepare?
How is the procedure performed?
Pelvic Ultrasound
An ultrasound machine uses high-frequency sound waves to produce images of the internal structures of the human body. Ultrasound of the pelvis is to visualize and assess structures and organs in the lower abdomen and pelvis.
How can I prepare for Pelvic Ultrasound?
No fasting is needed. You will need to keep a full bladder for the ultrasound of the pelvis.
How long does Pelvic Ultrasound take?
It will take about 15 – 30 minutes depending on the complexity of the scan.
Abdomen and Pelvic CT Scan
Computed Tomography (CT) is an examination that uses x-ray to produce images of the internal structure of the large bowel. The images are then reported by a radiologist.
How should I prepare for the procedure?
You should wear comfortable, loose-fitting clothing to your exam. You may be given a gown to wear during the procedure.
Metal objects including jewelry, eyeglasses, dentures and hairpins may affect the CT images and should be left at home or removed prior to your exam.
You may also be asked to remove hearing aids and removable dental work. You may be asked not to eat or drink anything for several hours beforehand, especially if a contrast material will be used in your exam. You should inform your physician of any medications you are taking and if you have any allergies, especially to contrast materials.
Also inform your doctor of any recent illnesses or other medical conditions, and if you have a history of heart disease, asthma, diabetes, kidney disease or thyroid problems. Any of these conditions may increase the risk of an unusual adverse effect.
Women should always inform their physician or technologist if there is any possibility that they are pregnant.
Abdomen and Pelvic CT Scan
Computed tomography (CT) of the abdomen and pelvis is a diagnostic imaging test used to help detect diseases of the small bowel, colon, liver, gallbladder, pancreas, kidneys, uterus, prostate and other internal organs CT scanning is fast, painless, noninvasive and accurate, performed with intravenous contrast material after the ingestion of oral contrast.
How Should I Prepare For The Procedure?
You should wear comfortable, loose-fitting clothing to your exam. You may be given a gown to wear during the procedure.
Metal objects including jewellery, eyeglasses, dentures and hairpins may affect the CT images and should be left at home or removed prior to your exam. You may also be asked to remove hearing aids and removable dental work.
You may be asked not to eat or drink anything for several hours beforehand, especially if a contrast material will be used in your exam. You should inform the doctor of any medications you are taking and if you have any allergies, especially to contrast materials.
Also, inform your doctor of any recent illnesses or other medical conditions, and if you have a history of heart disease, asthma, diabetes, kidney disease or thyroid problems. Any of these conditions may increase the risk of an unusual adverse effect.
Women should always inform the doctor or technologist if there is any possibility that they are pregnant.
Gastroscopy (OGDS)
Gastroscopy (OGDS) or upper endoscopy is performed by introducing a flexible fiberoptic scope through the mouth to visualize the oesophagus, stomach and the proximal part of the small intestine. Patients are usually sedated. Diseases like erosion in the oesophagus, peptic ulcer, gastritis and Helicobacter pylori infection can be easily diagnosed.
Indications For OGDS:
Colonoscopy
A fiberoptic colonoscope permits inspection of the entire large intestine by introducing a long flexible tube through the anus and rectum. Any abnormalities on the lining of the large intestine can be detected. The bowel must be specially prepared for at least 2 to 3 days prior to the examination to enable a proper examination.
Indications For Colonoscopy:

Life Care Diagnostic Medical Centre Sdn. Bhd. 200401034597 (673106-V)
Bangsar South
WhatsApp: 0122343610
1st Floor, Wisma Lifecare,
No. 5, Jalan Kerinchi, Bangsar South,
59200 Kuala Lumpur
Cheras South
WhatsApp: 01127213620
19A-2 & 19B-2, Block E, Kompleks Komersil Akasa,
Jalan Akasa, Akasa Cheras Selatan,
43300 Seri Kembangan, Selangor
Operating Hour:
Monday – Friday: 8.00am – 5.00pm
Saturday: 8.00am – 1.00pm
Sunday & Public Holidays: Closed

